|
I recently had a conversation with a good friend who has a family member with a serious illness. She told me that close friends of the family had called her in distress about this family member, as if she was expected to comfort them! This made me remember an article I read recently about “ring theory.” I sent this article to my friend and suggested she send it to all of her friends and family. It’s important information about how to cope with friends and family who are dealing with a crisis or death. I think it is so necessary to understand, that I wanted to spread the word to all of you. (It’s also been called the circle of kvetching, for those who can relate to the Yiddish term). Here is the original article:
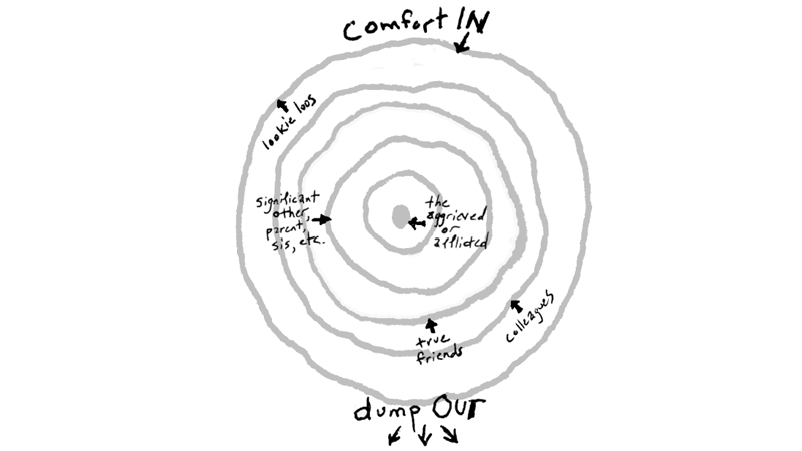
How Not to Say the Wrong Thing by Susan Silk and Barry Goldman Last year Elana Premack Sandler wrote this excellent explanatory article: Ring Theory Helps us Bring Comfort In by Elana Premack Sandler, LCSW, MPH A few years ago, psychologist Susan Silk and her friend Barry Goldman wrote a piece about a concept they called the “Ring Theory.” It’s a theory to help yourself know what to do in a crisis. If the crisis is happening to you, you’re in the center of the ring. If the crisis is not happening to you, you’re in one of the outer circles. Here are the basic tenets paraphrased from Silk and Goodman’s article:
The concept is simple: “comfort in, dump out.” I think disseminating this information will make the world a better place! It seems obvious when reading about the theory, but we have all likely been in the position of saying something similar that we later regretted. So please share this far and wide. As Susan Silk and Barry Goldman have said “And don’t worry. You’ll get your turn in the center ring. You can count on that.” As most of you know, I am a zealot for the overthrow of the healthcare “system”—since it is not adequately serving any of us. You might think overthrow is a bit of hyperbole, which I suppose it is, but I believe what we have now needs to be totally reworked, including how it is paid for. Putting patches on a sinking ship is too little too late.
An example of how badly this system—controlled by financial considerations—went off the rails has been in the news lately in Seattle. One of the major healthcare systems in our area underwent an expose by The Seattle Times; it seems the leadership of the neurosurgery department had lost its moral compass, and what was occurring was unethical and also illegal in some cases. Quality of care had been sacrificed for profit. A Lost Voice by Mike Baker Unfortunately, patients suffered poor outcomes and there was at least one death that likely could have been averted. Heads rolled, the head of the department lost both his job and his medical license, the CEO resigned, the state department of health investigated, JCAHO got involved (never a good thing), and major changes are underway. There are many fine doctors in this hospital system, and I was extremely gratified to learn that many in that department, many of whom I have worked with, very vigorously objected to the circumstances and some suffered repercussions (one just was awarded a large amount of money for being fired as a whistle blower!). The past chief executive of the system’s physician division confronted the leadership regarding the situation suggesting that action be taken. So why am I writing about this? For one, it confirms what I know to be true—most doctors are committed to doing what is right for their patients, do it well, and call out those who are acting counter to their principles. For another, when I initially read the articles in the paper about this investigation, I was screaming in my head “no, you need an advocate there!” A young woman lost her life, despite the fact that her father is a doctor and was present in the ICU urging those caring for her to do what was needed. His concerns went unheeded. Having someone who is not related to the patient serving as an advocate is invaluable. No one can think clearly when their child is struggling to breathe. As advocates, we have no qualms about raising a ruckus, confronting care givers, or going up the chain of command until we get what is needed, particularly when it is a life-threatening event. I would like to believe that if an advocate had been there this young woman would still be alive; I don’t really know if that is the case, but I do know that if I had been there, there would have been a lot more yelling and screaming going on. Sometimes that is the best thing an advocate can do. On that less than uplifting note, I do hope all of you had some rest and enjoyment over the holidays and are having a wonderful new year. I am something of a zealot for extolling the values of community and the need for personal connection. In my work as a healthcare advocate, I find myself urging new or established advocates to join the organizations for advocacy and to attend the conferences. I belong to 3 such organizations: National Association of Healthcare Advocacy Consultants, Washington State Health Advocacy Association, and the Alliance of Professional Health Advocates. It is worth every penny!
Why? Talking to your peers is invaluable in any profession, and in our line of work, there aren’t all that many of us. We get support, validation, and knowledge about our field when we meet and network with each other. This newsletter is about having a support network, building community, and more. It is about improving the quality of care for our clients, smoothing transitions, and getting business at the same time. I have wonderful advocacy colleagues around the country, but was recently reminded of the value of connection because of a circumstance with a fellow advocate and her client. My colleague, Dianne Savastano, is the founder and principal of Healthassist, a healthcare advocacy firm based in Massachusetts. Dianne had worked with a member of a family on the east coast. When the father, who was living in Seattle at the time, began having health issues that were not resolving, the family asked Dianne if she had anyone in Seattle like her. She readily said that she did, and I was promptly connected to the father in Seattle. This began a very pleasant and rewarding several months working with my client, whose goal stated at the outset was to move back to the east coast (besides resolving his health issues). We were able to make tremendous headway on the health issues, and only had to delay his move once. And of course, Dianne and her associate, Anne Jacoby, sprang into action to make the move a carefully thought out and smooth transition, putting all the pieces into place on the east coast. This is the ultimate in coordination of care. I can completely relax knowing he is in the best of hands. Not to mention giving a shout out to his wonderful family both here in Seattle and on the east coast; they are the ultimate community and make it all possible! This has been such a good example of the value of connection and the reason for community building that I will continue to promote it. I will do whatever I can to give the best service to all of my clients, while continuing to network and connect with my fellow advocates. As Helen Keller once said, ”We cannot accomplish all that we need to do without working together.” I have been thinking a lot about end of life planning. I recently started helping people with this aspect of their lives by acting as a healthcare power of attorney for those who need a non-family member in that role. And yes, I intentionally italicized "of their lives."
A good friend’s mother recently died at age 94; she was well loved by her family, and very well cared for despite living for many years disabled by a stroke. My friend and his family were able to be with her in an inpatient hospice setting, it was clear she did not want any extraordinary measures taken to prolong the inevitable, and they could sit and hold her hand as she passed. Sounds pretty ideal, right? And despite glitches along the way, it seems so. As we were discussing it after her shiva (the Jewish period of 7 days of the acute phase of mourning—or less depending on your adherence to classic protocols), it occurred to me that there are 3 general death scenarios. The one above is the clear scenario that most of us envision as “a good death”. Putting in Place An A-Team of Allies by Judith Graham Another scenario is where a family member dies suddenly, unexpectedly, and the family and friends are left in shock, having had no time to process it before it happens. Interestingly, this is not necessarily a “bad death” for the deceased, but it certainly is hard for the family. Don't Wait: Now's the time to discuss end-of-life-care by Robert Powell The third general scenario is where some or all of the participants (including the “patient”) have not accepted that death is a part of life (thus the italics above). The hard discussions of what the person wants at the end of life, when they want to push on, when they want to call it quits, where they want to die, who they want with them—all of the factors that go into a “good death”—have not been discussed, or the family ignores the wishes and countermands them. Or worse, there is disagreement among family members about the treatment course. Why you need a Healthcare Proxy and how to choose one by Debbie Reslock I cannot claim to have the lock on what a good death looks like to others, but I do know what can be done to lessen the stress felt by families going through this passage. In the first scenario, end of life wishes were known and discussed, and it was the end of a good long life. In the second scenario, there was likely no preparation, and nothing can mend the shock felt by the family except time. In the third scenario, there is a lot of preparation that could be done to prepare for and avoid conflict and stress. This is why I advise everyone to have a healthcare power of attorney designated and an advance directive in place. We can make a death better for both the patient and the family if we confront this before it is needed. I have been through two of the three scenarios personally, and I vastly prefer the first one. As spring has arrived, I have been immersed in something that involves the end of things rather than the beginning. Recently, I started a new service helping people plan for what they want at the end of their lives (i.e. helping them figure out what they want in their advance directive), while also serving as the healthcare power of attorney for those who do not have or do not want a family member to do so. Writing this newsletter was spurred by an article I read recently by an attorney—no longer practicing—who holds the position that lawyers have no business in the field of advance care planning. Lawyers have no business in the field of advance care planning by Phyllis Coletta The author of the article, Phyllis Coletta, says: Here’s what happens when a lawyer gets involved in advance care planning: They tell you to appoint a health care agent, but don’t stress that you must talk to that person and all other loved ones about your values and range of decisions. And: My ER doc friends tell me there is no document that comes close to the help of a well-informed family at the bedside. I often tell people that I thought my family was the norm in terms of advance care planning. (Why I thought this was the case is a mystery to me!) My parents had a very thorough advance directive, which we all had copies of, and we all knew who the agents in charge were. When crises occurred, we could read the document to figure out what each parent wanted for their care. Further, my siblings and I are very close to each other and would talk frequently to ensure their needs were being met. Also, my parents had arranged for themselves financially, which reduced the burden on us as their children. When I began researching this kind of work, I was surprised by what I found. I was astonished that potential clients did not realize that I needed to spend quite a few hours with them to get to know them, and what they would like to happen if they are unable to speak for themselves. In fact, I tell them that I am channeling them, so it is important to know who I am channeling! Isn’t that what we all want—someone who will carry out our wishes as close to what we would do for ourselves as possible? What have I found instead?
I want to leave you with some really great resources for figuring out your or your family’s end of life decisions: 5 wishes https://www.agingwithdignity.org/ gyst.com https://www.gyst.com/ death over dinner http://deathoverdinner.org/ the conversation project http://theconversationproject.org/ This is a conversation that does not need to be painful, sad, or morbid. It can create connection, and avoid a lot of pain in the end! Happy holidays to all of you!
This is a good time of year to look back at the year and do a survey of how well we are accomplishing our goals. I’ve been thinking about how to spread the word about healthcare advocacy, and this story struck me as a case in point. Recently a colleague and friend said to me that she had thought about calling me (as a healthcare advocate) when her son had been very ill. He was much better now, but the family had gone through a very difficult and scary time. I wondered what had made her hesitate while they were going through the health crisis. We met for lunch recently, and she told me the story. Here it is with many identifiers changed, and I’ve included my comments in italics where a healthcare advocate would have helped. This 22-year-old male’s past medical history is significant only for migraines, he has been active in sports and has been routinely healthy. He joined a fraternity in college and then moved into a house with friends where he began to have respiratory illnesses, and his health began to deteriorate. The house, which his mother describes as a dump (I thought that the house my son lived in his fourth year of university should be burned down when they moved out), was subsequently found to have black mold. He developed gastric ulcers that eventually bled and he was treated according to the appropriate protocol. In December of 2014, he called his mother during a particularly bad respiratory infection to “come get me”. She did, and he was found to have pneumonia. Due to his illness he had to take an extra semester to graduate, but he recovered at home with appropriate medical care and finished school in March of 2015. In October of 2015, his family noted that he was becoming more and more irritable, and he began to have more and more fatigue. (I should add here: this would not necessarily trigger a call to an advocate, but it would have been a good time for him to see his primary care doctor). Within 2 months he was sleeping more and more and eating less and less (again, see your doctor! This is not normal!). In January of 2016 he noticed blood in his urine. Was this a urinary tract infection? He saw a urologist, who also ordered a CAT scan, which was normal. The possibility that he had passed a kidney stone was considered, although the symptoms were not particularly characteristic for that, and my friend’s son did not think that it was likely. A week later his nausea, irritability, and fatigue had markedly increased. He saw a nephrologist at his medical clinic, who wondered if it was a virus. A creatinine was checked (this measures kidney function) and it was found to be 3.5 (abnormally high, especially for a young person). He was scheduled to have a scope of his bladder, but that was cancelled due to respiratory symptoms (asthma?). The next day, when he saw his urologist his creatinine was 5.5 (even worse! And rapidly worsening!) It was clear that something was going on that needed to be addressed urgently, and he was admitted to the hospital—and put on the oncology floor! Here is the first point where a healthcare advocate would have been helpful. The family felt lost in space. And he was on an oncology floor! An advocate could have helped with the communication between the medical team and the family, and explained that this did not mean he had cancer. At a time like this, someone who can keep track of all the pieces of information and relay them calmly to a very distressed patient and family can be priceless. He proceeded quickly to a diagnostic workup that led to the diagnosis of a rare autoimmune syndrome that attacks the kidneys. As a kidney biopsy confirmed this, his creatinine climbed close to 7, and his blood pressure increased. The doctors immediately began treatment with plasmapharesis (a method of removing blood from the body, separating the components, and reinfusing the cells but not the plasma--a way of getting rid of unwanted antibodies). They also treated him with prednisone, as well as an oral chemotherapeutic agent. He was told that 50% of his kidney tissue had been affected by the immune complexes. He believed, wrongly, that he was destined for a kidney transplant, and soon. Next place for an advocate to intervene: not all medical providers communicate well with patients, and making sure the patient and family have a realistic idea of what could lie ahead is important. The emotional distress that this misinformation caused was significant, and entirely unnecessary. He continued to have daily plasmapharesis for 4 weeks; his hospital stay was complicated by the development of a blood clot in his arm that required IV anticoagulation (overtreatment led to him bleeding from everywhere but dissolved the clot very rapidly), and a bout of hospital acquired pneumonia after about 2 weeks was treated with IV and oral antibiotics. One of his doctors took his pathology slides to a conference because it was so unusual. He was discharged after a 4-week hospital stay on 20 different medications. His creatinine is now around 1.5. What went well?
A healthcare advocate would have been able to work with the system and the patient to be sure he had some mental health consultation during the hospital stay. In addition, the family needed some support, and this also could have been facilitated. In addition, if the nephrologist is going to change weekly, the healthcare advocate can be the continuity to be sure all sides are hearing each other. Now: He is recovering at home, rides his motorcycle, and doing much better. He is off of chemo and has weaned down his prednisone. He has gotten much feistier (he doesn’t want his mom going to doctor appointments with him). But he went through a significant period of depression, and was even suicidal. He is on an antidepressant, which helps. He still feels under the influence of “chemo brain”, but this is slowly improving. And he is experiencing what sounds to me like PTSD. A healthcare advocate would stay involved after discharge from the hospital, and perhaps could have hastened treatment for the depression, as well as help find resources to treat PTSD. As my friend said, a healthcare advocate is like a SWAT team that can swoop in and make sure everything that needs attention gets attention. My friend’s son had a fairly rapid diagnosis, good medical care, and is doing much better. Even so, the journey could have been so much less painful, scary, and a much smoother ride with an advocate. A healthy new year to all! I hope you are all having as glorious a summer as we are having in Seattle. Its sunny, green, and a great temperature! I have been dreaming and having frequent conversations lately about a better way forward — for healthcare, our planet, and human relations in general. One of the issues that is often raised about our healthcare system is that the voice of the patient is lost, and this is definitely a focus of healthcare advocates. Narrative medicine is a discipline that has arisen to address this. Wikipedia defines narrative medicine as follows: Narrative medicine is a wholesome medical approach that recognizes the value of people's narratives in clinical practice, research, and education as a way to promote healing. Columbia University Medical Center Program in Narrative Medicine describes the program by saying it “fortifies clinical practice with the narrative competence to recognize, absorb, metabolize, interpret, and be moved by the stories of illness.” The fact that such a respected university has a program in Narrative Medicine shows that this field is gaining traction, as well it should. The story used to be a primary concern; now we have to name a new discipline in order to bring it back. What is intuitively clear is that feeling that we are heard feels much better than not, and there are studies that show how this impacts our healing. Additionally, listening to the story can be lifesaving. Here is an article describing an incident that, while not lifesaving, was tremendously impactful in terms of preventing injury and pain. An Avalanche of Data Buries the Patient Story by Rob Lamberts, MD I was really anxious. My father’s legs were getting weaker and his pain was worsening. He had been having pain for quite a while, and that pain was often disabling in its severity, but the weakness was alarming.... Read more. As “modern medicine” evolves, the amount of data available has grown exponentially. Narratives are increasingly neglected in favor of facts and figures, thought to be more scientific and objective. I cannot disparage all the knowledge we have gained, but the stories and our sense of human connection, “seeing” our patients and clients, cannot be sacrificed in its favor. Here is a great story from Intima the Journal of Narrative Medicine written by a professor at the University of Washington, Josephine Ensign, an adjunct associate professor and a leader in the field of narrative medicine. Medical Maze
by Josephine Ensign Late one November night in 2000, I drove myself to the ER at the UW Medical Center... My legs had been tingling and getting progressively benumbed over the past week. The numbness started in my toes and now reached my butt and groin region, plus my toes were turning blue..... Read more. The take home message from this article is clear. We need supportive data, but we also need the patient narrative. Both are critical to health and healing, and something important will be lost if we ignore either one. If you'd like to hear more from Josephine Ensign, she will be a speaker at the National Association of Healthcare Advocacy Consultant’s (NAHAC) National Conference in Seattle, November 16 - 18th, where we will be focusing on narrative medicine and interaction for the first afternoon. For more information about the conference, including additional speakers and registration, please visit the NAHAC website. Next month, join me as I take a look at integrative medicine, another discipline that focuses on the patient / physician relationship, and is not well understood by most people. Happy summer everyone. I am relishing the beautiful weather and flowers, as well as the fresh vegetables and long hours of daylight! I have been thinking a lot recently about how things are not always as they appear; often you need to dig a little deeper to find out the truth. So much of what we read these days is hype or selective reporting. Sadly, this is extremely true of medical information. I recently read an article about how Big Pharma (the pharmaceutical industrial complex) has made this into an art of sorts, and that if you take what you hear at face value, often you will be deceived. More importantly, this topic came to mind because of an article that has received a tremendous amount of press in the media after it was published in the British Medical Journal. Medical Error - The Third Leading Cause of Death by Martin Makary and Michael Daniel Dr. Martin A. Makary of Johns Hopkins and research fellow Michael Daniel wrote a paper stating that medical error is the third leading cause of death in the US. This is quite alarming, and in medical circles has led to quite a bit of head scratching—this is not what any of us have experienced, so is it really the case? How could we be so unaware of the third leading cause of death? Prior to this paper the data used to discuss rate of death from medical errors was from 1984. Dr. Makary does state that the 1984 study was not great science, however, they did find several good studies, reviewed the data, and came up with the figure of 251,000 deaths per year in the US from medical error. It has been pointed out that Dr. Makary used 4 observational studies on incidents that occurred between 2000 and 2008, not exactly an accurate reflection of what the rate is now. More importantly, the patients in those 4 studies were dominated by inpatients in the Medicare community, a more risk prone group than the general public. In fact, the authors say “the assumptions made in extrapolating study data to the broader U.S. population may limit the accuracy of our figure”. Aha, maybe it’s not as accurate as it appears in a splashy headline in our newspaper. Check out the analysis and rebuttal of the science in the article below. ANALYSIS - Re: Medical Error - The Third Leading Cause of Death by Kaveh G. Shojania Cause of death is often multifactorial; a terminally ill patient may experience a medical error, but their underlying disease may be the majority of the cause of death. There is a huge and often unrecognized difference between an error and a bad outcome. All medical treatment has a risk of bad outcome even when no errors occur. This is summed up very well in an article from Vinay Prasad on Stat News. "While the report in the BMJ — and the press release promoting it — sounded like researchers were on to something new, they were merely reminding us of old data." Don't Believe What You Read on New Report of Medical Error Deaths
by Vinay Prasad No one would disagree with the efforts to eliminate medical errors to the highest degree possible, and like many important aspects of healthcare, this is one that is underfunded, understudied, and often swept under the carpet. Yet, to overstate the incidence does not help the effort to decrease medical error. As advocates we will never stop working to prevent medical errors from occurring, but we need to be careful not to see them around every corner where they may not exist. Happy spring everyone! Here in Seattle the weather is unseasonably gorgeous, and it makes everything better. This is the last newsletter where I will focus specifically on upstreamists, and I want to do so around a theme: end of life planning. I would bet most of you don’t know that April 16th was National Healthcare Decisions Day (NHDD). From their website: “National Healthcare Decisions Day(NHDD) exists to inspire, educate and empower the public and providers about the importance of advance care planning. NHDD is an initiative to encourage patients to express their wishes regarding healthcare and for providers and facilities to respect those wishes, whatever they may be. The theme for 2016 is "It Always Seems Too Early, Until It’s Too Late." "NHDD exists as a 50-state annual initiative to provide clear, concise, and consistent information on healthcare decision-making to both the public and providers/facilities through the widespread availability and dissemination of simple, free, and uniform tools (not just forms) to guide the process. NHDD entails 50 independent, but coordinated, state and local events (necessitated by the difference in state laws and dynamics) supported by a national media and public education campaign. A key goal of NHDD is to demystify healthcare decision-making and make the topic of advance care planning inescapable. On NHDD, no one in the U.S. should be able to open a paper, watch TV, view the internet, see a physician or lawyer, or go to a healthcare facility without being confronted with the topic of advance care planning. Among other things, NHDD helps people understand that advance healthcare decision-making includes much more than living wills; it is a process that should focus first on conversation and choosing an agent." I am aware that it seems incredibly onerous to sit down and think about end of life planning, but there are a lot of resources out there to simplify it. In Washington State, you don’t have to have a lawyer to sign a Healthcare Power of Attorney document (aka healthcare proxy)—in fact you don’t even need a notary. You can go online, get documents, print them out, fill them in, and give them to your loved ones! Please do this for the sake of those you care about if not for yourself. And now for the upstreamists. The people and organizations I am going to highlight are all working to make this subject accessible to everyone, not just lawyers. The goal is to change the thinking of our society that this is just not something to talk about, or that there will be time later, but rather to take action now so that your individual wishes can be known. The first organization I want to mention is Get Your Sh*t Together, founded by Chanel Reynolds. She founded the organization after the tragic and sudden loss of her husband in my neighborhood! Here is the story from the New York Times. This is a stunning example of “it always seems too early until its too late”. A Shocking Death, a Financial Lesson and Help for Others by Ron Lieber The next organization I want to feature is Death over Dinner, started by Michael Hebb, who found out about the difficulty of helping those at the end of life when he met two doctors on a train ride. The doctors were dismayed about our healthcare system and relayed this startling fact: Nearly 75% of Americans want to die at home, yet only 25% of them do. His organization makes it almost fun to have these conversations: "Send an invite to loved ones, and then set the table to start talking about end-of-life care and how we want to live the final days of our lives. We'll provide the tools and tips to get the conversation started. You choose the guests and the menu, and let the conversation and the wine flow." Michael Hebb on TEDMED ~ What Happens When Death is What's for Dinner And finally, The Conversation Project began in 2010, when Ellen Goodman, a well known journalist, and a group of colleagues and concerned media, clergy, and medical professionals gathered to share stories of “good deaths” and “bad deaths” within their own circle of loved ones.
Over several months, a vision emerged for a grassroots public campaign spanning both traditional and new media that would change our culture. The goal: to make it easier to initiate conversations about dying, and to encourage people to talk now, and as often as necessary, so that their wishes are known when the time comes. All of these sites have easily accessible documents for anyone to use. And I would be remiss if I didn’t mention The Five Wishes from Aging with Dignity, a website that offers downloadable living wills that help document and describe your desires for end of life care. If you want any more information, let me know. Your family and your doctors will thank you. Happy almost spring, although many of you are still being hit with snow and ice! I want to continue the theme I began 2 months ago where I discuss “upstreamists”, those who are “going upstream” to find the cause of problems in our healthcare system, and then working directly to create change. Last month I profiled Health Leads, a nonprofit organization that is providing information and connection for low-income patients, as well as providing access to many wrap-around services that affect health and wellbeing, such as having adequate food, transportation, and heat in the winter. Yesterday I had a very stimulating conversation with a young physician who had just finished medical school in the UK. He felt drawn to medicine by his desire to help others, like most doctors, but he did not gravitate to a particular specialty. Instead, he’s been traveling around the US talking to upstreamists in order to tap into their experiences. His network includes those that create technological tools that try to fix some discreet dysfunctional piece of healthcare, rather than affecting the whole system. All of the projects he told me about were lovely little gems. But there is a problem with creating beautiful gems. When you have something that is rotten underneath, applying beautiful gems to it does not cure the problem; it remains rotten. We need to look deeper to figure out what we can do to impact our healthcare system, from the inside out. Dr. Rushika Fernandopulle of Harvard University, is doing just that with Iora Health. I’ve been following him for a number of years. Here is what Iora Health says about itself: We’re changing health care from the ground up. We believe better health care starts with better primary care. Our simple yet radically different approach to restoring humanity to health care is three-fold: Team-based care that puts the patient first, a payment system based on care, not billing codes and technology built around people, not process. ………. Our care team, which includes a dedicated advocate for each patient, works together to treat the whole person. We see people when they’re sick, but also when they’re well, so that we can keep them healthy. Here, the environment is caring and patients have a voice. It’s our job to give them everything they need to live happier and healthier lives. Here is a fabulous and inspiring talk by Dr. Fernandopulle, who discusses how and why we need to change the healthcare system. And a freebie thrown in: The Hot Spotters is the seminal article on change in the healthcare system, by Dr. Atul Gawande, published in the New Yorker. This is a must read in my opinion, to know where the “rot” is. It would not be an exaggeration to say that this article changed my life.
|
AuthorDr. Sima Kahn muses on being a healthcare advocate, the troubles with our healthcare system, and how to advocate for ourselves. Archives
August 2021
Categories
All
|

 RSS Feed
RSS Feed